TMS for Functional Movement Disorder (FMD)
A cutting-edge approach to disrupting the abnormal motor patterns created by disrupted brain-body signaling — without medications or surgery.
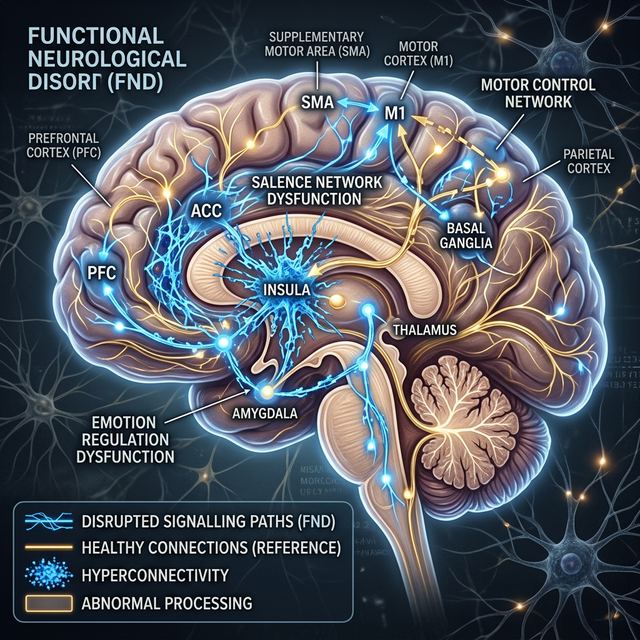
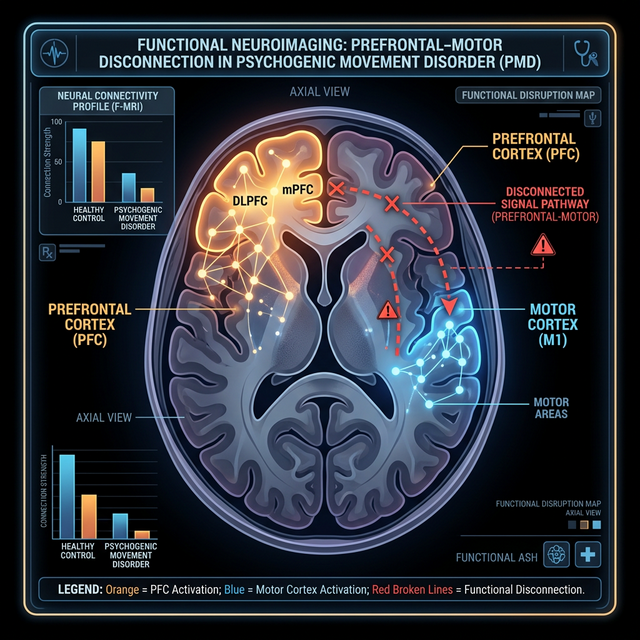
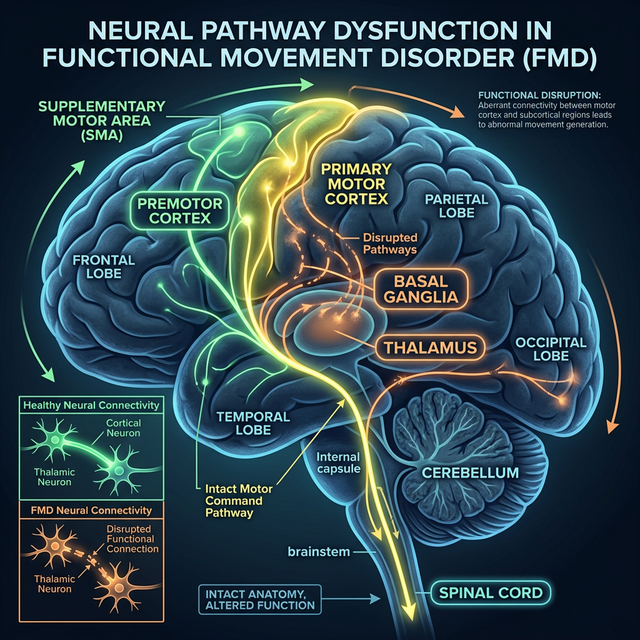
Functional Movement Disorder is a condition in which the brain produces abnormal, involuntary movements — not due to structural damage, but due to a disruption in how brain networks communicate with each other. Patients experience real, often disabling symptoms: weakness, abnormal gait, tremors, and jerks that cannot be explained by conventional neurological disease.
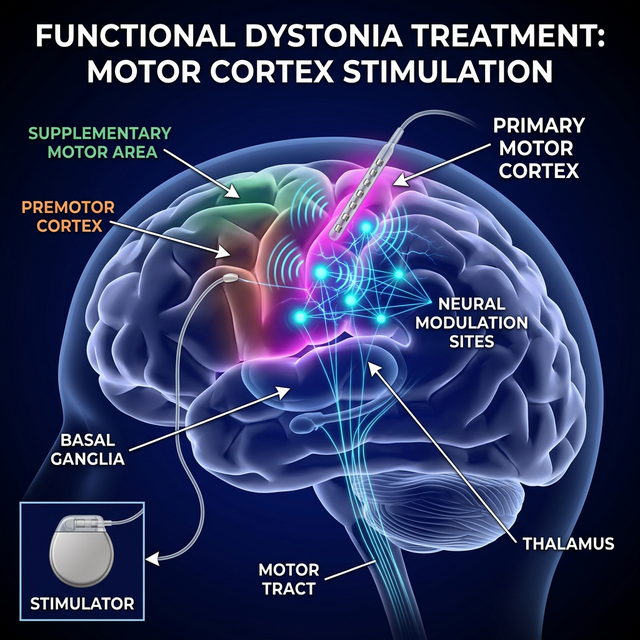
TMS offers a targeted intervention at the root of FMD — the motor cortex and supplementary motor area. By delivering focused magnetic pulses, TMS can interrupt maladaptive motor patterns and help the brain re-learn normal movement control, leveraging the brain's capacity for neuroplasticity.
Dr. Amin uses motor cortex mapping to identify the exact circuits driving dysfunctional movements, ensuring every TMS pulse is targeted precisely to the source of disruption.
Symptoms TMS can address in FMD:
Abnormal Gait
Unusual or dragging walking patterns that have no structural cause but originate in miscommunicating brain circuits.
Functional Weakness
Loss of motor control or limb weakness with normal neuroimaging, caused by disrupted motor network signaling.
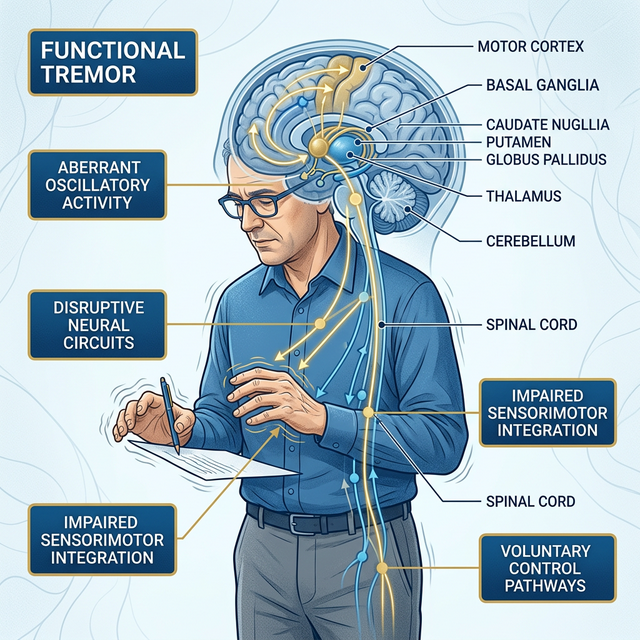
Myoclonic Jerks
Sudden involuntary muscle spasms that are functionally-driven rather than caused by epileptic or organic disease.